 The NHS’s ‘Safe and Sustainable’ review of the 11 children’s heart surgery units in England has recommended a reduction in the number of units to create fewer, larger centres.
The NHS’s ‘Safe and Sustainable’ review of the 11 children’s heart surgery units in England has recommended a reduction in the number of units to create fewer, larger centres.
It has put forward four options for a four-month public consultation period completing on 1 July 2011, with the LGI unit featuring in only one option.
An on-line petition has been set-up http://www.thepetitionsite.com/6/help-to-save-ward-10-childrens-cardiac-lgi/ that now has over 20,000 signatures.
Option A – seven surgical centres
Freeman Hospital in Newcastle Alder Hey Children’s Hospital in Liverpool, Glenfield Hospital in Leicester, Birmingham Children’s Hospital, Bristol Royal Hospital for Children with 2 centres in London
Option B – seven surgical centres
Freeman Hospital in Newcastle, Alder Hey Children’s Hospital in Liverpool, Birmingham Children’s Hospital, Bristol Royal Hospital for Children, Southampton General Hospital with 2 centres in London
Option C – six surgical centres
Freeman Hospital in Newcastle, Alder Hey Children’s Hospital in Liverpool Birmingham Children’s Hospital Bristol Royal Hospital for Children with 2 centres in London
Option D – six surgical centres
Leeds General Infirmary, Alder Hey Children’s Hospital in Liverpool, Birmingham Children’s Hospital, Bristol Royal Hospital for Children with 2 centres in London
London – The preferred two London centres in the four options are:
Evelina Children’s Hospital and Great Ormond Street Hospital for Children
Comment from Andrew Jones, MP for Harrogate and Knaresborough:-
“ If this unit was to close it would mean that families would be left with no option but to travel long distances to specialist units in Birmingham, Leicester, Newcastle or Liverpool. At times of great stress and where minutes matter this is not a practical option for families in this constituency.
I highlighted the importance of the unit at a recent debate in the House of Commons. The government review needs to consider the distance to the heart units for children with congenital heart disease and for their families. Provisions also need to be made for long-term support for families who when dealing with sick children are under very great pressure. The LGI ticks all the boxes providing 22 rooms for families to stay while visiting their sick children and is ideally situated to serve Yorkshire and the neighbouring counties, within two hours drive for nearly 14 million people. That is why this unit must stay open.”
The link to the North Yorkshire MP’s House of Commons debate on children’s heart surgery in Leeds is as follows: http://www.theyworkforyou.com/debates/?id=2011-03-03b.533.0
A story from one of the families effected
Allison Mace lives in Harrogate and is the Grandmother of Georgia who is now 5. The words here are Allison’s own words and we felt they should be left as they were written:-
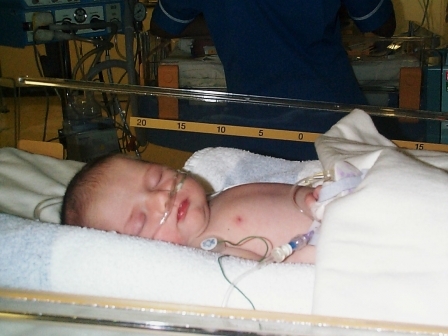
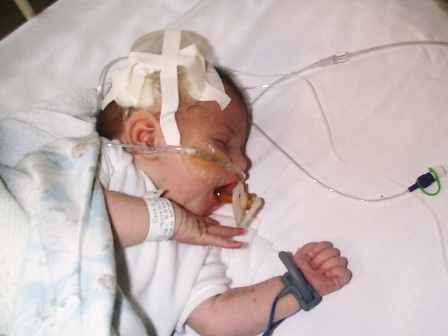 On the 17th February 2006 Georgia was born and was discharged home a day later. When Georgia was 5 days old she collapsed at home – the diagnosis was Heart Failure. We were rushed to Harrogate District Hospital and awaited a medical team coming from the LGI to transfer her. On arrival at LGI the prognosis was not good, after doing tests they found she had an Interrupted Aortic Arch, 2 VSD’s (holes) and Valve Stenosis. It was doubtful that she would survive. She was so poorly they couldn’t operate straight away and we she was admitted to the Neo Natal unit first and put on drugs and life support to allow her to rest for the hike ahead. We were given parents accommodation so that we could remain by her side.
On the 17th February 2006 Georgia was born and was discharged home a day later. When Georgia was 5 days old she collapsed at home – the diagnosis was Heart Failure. We were rushed to Harrogate District Hospital and awaited a medical team coming from the LGI to transfer her. On arrival at LGI the prognosis was not good, after doing tests they found she had an Interrupted Aortic Arch, 2 VSD’s (holes) and Valve Stenosis. It was doubtful that she would survive. She was so poorly they couldn’t operate straight away and we she was admitted to the Neo Natal unit first and put on drugs and life support to allow her to rest for the hike ahead. We were given parents accommodation so that we could remain by her side.
10 days later came our first proper experience of how fantastic the doctors and medical team at Ward 10 actually are.
We moved to Ward 10 in preparation for Georgia having her surgery to repair the Interrupted Aortic Arch and VSD’s. Her specialist Dr John Thomson from the start was brilliant and although could give no promises was always very honest and supportive and made clear they would do everything they could for her. At the same time the nurses and other medical staff were always caring and supportive of our needs and the care for Georgia was excellent. They are all highly trained and very experienced.Georgia underwent a nine hour operation at the skill of her surgeon Mr Weerasena, and the op was successful. She then began a slow but positive recovery in the Paediatric Cardiac Intensive Care Unit Again the staff are so highly skilled and trained and again although very busy always had time to talk to you and answer questions or concerns and you know that by how they work that they are all really dedicated. Once back on Ward 10 the doctors and nurses gave us back the confidence to begin caring for Georgia after such an emotional and wrenching beginning. She was discharged on 13th March 2006
I wish this had been or only experience of Ward 10 but unfortunately it wasn’t.
On the 22nd April 2006 Georgia had a massive collapse, she was retrieved from Harrogate Hospital by the Ward 10 medical teams and very impressively by John the Consultant Anaesthetist from the Cardiac Intensive Care Unit who sped to Harrogate on his motorbike to try and stabilise her. Time really was an issue. On his arrival her condition was very poor and she had severe Acidosis.
On her arrival back at LGI things looked very bleak. She had multi organ failure and it was expected she wouldn’t survive the night. Again we were given parents accommodation and at around 1am the Ward Sister rang our room and said we should sit with Georgia as she was deteriorating , they arranged for the hospital vicar to come to see us at our request and he gave Georgia a blessing. Remarkably she hung on and although didn’t improve she didn’t leave us either. She remained like this for 48 hours. Dr Thomson then did another procedure on her called a Balloon Aortic Valvuloplasty to stretch the Valve Stenosis. She began to improve and was eventually moved back onto the main ward. She was discharged home on 12th May 2006.
The care of the staff both to Georgia and ourselves was first class and we will never be able to thank them enough for what they did for Georgia and us. And as for the retrieval team and John on his motorbike I feel there is absolutely no doubt that had they had to come from further away or had Georgia had to be transferred further than the LGI then the little girl who is so precious to us and who had her 5th birthday this year would not be here now.
On a number of occasions I have rung the ward and been able to talk to the doctors and have been able to take Georgia in to be checked over when we have had concerns. They have always been very understanding and the care they show is open ended
In January this year Georgia underwent another Balloon Aortic Valvuloplasty as she became poorly over Xmas.
She has other health difficulties and some learning and behaviour difficulties and is a very difficult patient as she is petrified as soon as you approach Leeds but Dr Thomson and the nursing staff are always patient with her both on the ward and in outpatients.
She still has another major op to have to replace the Heart Valve that is affected by the Stenosis and I shudder to think what will be the out come if the Unit at Leeds closes and it needs to be done in an emergency and she has to rely on Newcastle or Birmingham. Also at traumatic times like this you need your friends and families to lean on and gain strength from and that’s impossible so many miles away.
If you wish to show your support then:-
sign the petition http://www.thepetitionsite.com/fb/6/help-to-save-ward-10-childrens-cardiac-lgi/
Lobby your local MP





An incredible but not uncommon story; very touching when you have been part of it yourself as I have been with my daughter (Emma) who is now 28 years old – but still attending LGI and yes, she still requires further corrective sugery when she is deemed ‘ready’ even though she has had 4 majors so far!. To consider the closure of Ward-10 is just unimaginable in every sense of the word and I seriously question as to just what planet these decision makers are on and likewise ask, Do they listen to the public? If the recent general meeting re the closure is anything to go by then the answer is No. They completely ignored ALL public generated questions. My simple question relating to the potential closure is, Will the Ward-10 Consultant(s); Doctors and nursing staff be made redundant? Do any of these people understand the stress levels; the necessity to drive under same and more to the point, the children themselves who will be going through an horrendous unknown experience. God Bless all the children and staff associated with Ward-10.